Table of Contents
- Durable Medical Equipment 101
- What is durable medical equipment?
- What does Medicare cover?
- What do other insurers cover?
- How much does DME cost?
- Who pays for DME?
- What if I need help with DME?
- Conclusion: DME is freedom if you learn how to fight for it
Durable medical equipment isn’t extra. Its not a luxury, and its not an add on to your care plan. In the real world, durable medical equipment (DME) is often the difference between living your life on your own terms and being trapped by your diagnosis, your finances, or your ZIP code. Ive seen too many patients discharged with a thick stack of papers and zero practical guidance on how to actually get the wheelchair, hospital bed, or oxygen equipment they were told they needed. That’s why any honest durable medical equipment 101: what it is, what it costs, and who pays for it article has to start with this blunt truth: the system is confusing on purpose, and if you don’t learn how DME really works, you will probably overpay, wait too long, or go without.
Ive watched families in Florida argue at the pharmacy counter about a walker that insurance should cover, and Ive sat at kitchen tables going line by line through Medicare rules trying to figure out why one hospital bed is covered and another isn’t. The good news is that once you understand the rules of the DME game what qualifies as DME, how Medicare and commercial insurance think, and when Medicaid or waiver programs step in you can push back, appeal, and plan ahead instead of accepting no as the final answer. Lets walk straight through it, without sugarcoating and without the usual vague advice.
Durable Medical Equipment 101
Learn durable medical equipment 101 what DME is, how much it typically costs, and who pays so you can plan care and finances. – Durable medical equipment (DME) are prescribed, reusable home medical devices like wheelchairs, hospital beds, oxygen systems, walkers, and CPAPs that support mobility, breathing, or daily living. – Medicare Part B covers medically necessary DME (typically 80% after the Part B deductible with supplier and prescription rules), while Medicaid and private insurers vary and often require prior authorization or limit rentals vs. purchases. – Costs range from under $100 for basic supplies to thousands for complex devices, and payment can come from Medicare, Medicaid, VA benefits, private insurance, out of pocket, or assistance programs and payment plans depending on eligibility.
What is durable medical equipment?
Durable medical equipment is much more specific than anything medical you use at home. Insurers and Medicare use a tight definition: durable, reusable devices that you can use at home to treat or manage a medical condition, typically for at least three years. If an item doesn’t check those boxes, the chances of getting it covered drop quickly.
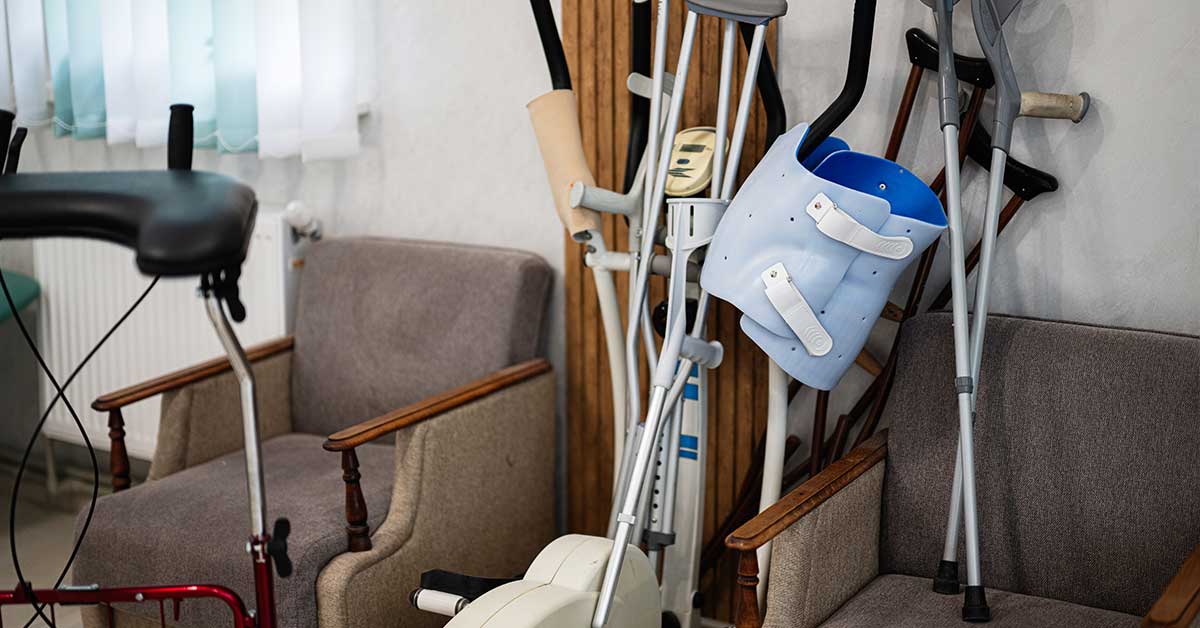
In practical terms, DME includes things like:
- Hospital beds and bed accessories
- Wheelchairs (manual and power) and scooters
- Walkers, rollators, and crutches
- CPAP and BiPAP machines for sleep apnea
- Oxygen concentrators and related supplies
- Nebulizers
- Patient lifts and transfer devices
- Commode chairs and certain shower chairs
- Some specialized pediatric equipment and adaptive devices
A good local provider like a full service durable medical equipment supplier will usually draw the line between DME and consumable supplies (like adult briefs, gloves, or dressings). That distinction matters, because rules and payers are often completely different. In my own experience helping families, the biggest early confusion is someone assuming their incontinence supplies are DME and must be handled like a wheelchair claim. In reality, those items usually fall under consumable medical supplies, with separate coverage rules and vendors.
DME also has to be medically necessary and primarily for use in the home. That last phrase is not a technicality. Its why Medicare will cover a standard power wheelchair for someone who cannot get around their house without it, but wont pay for a scooter just because they want to shop more comfortably at the mall. Ive seen doctors write well intentioned but vague prescriptions like scooter for community mobility, and the claim gets denied because the note ignored the in the home standard that Medicare and many insurers still cling to.
Insider Tip (DME Coordinator, 15+ years): If the equipment isn’t expected to last at least three years, assume its not DME and ask whether its a consumable, rental, or short term rehab item. The category determines who pays not the doctors preference.
What does Medicare cover?
Medicare is simultaneously the most predictable and the most frustrating payer for DME. The rules are written down, updated regularly, and fairly transparent. But they’re also rigid, slow to change, and sometimes completely detached from modern technology. Nonetheless, if you understand the framework, you can often anticipate denials and fix them before they happen.
Medicare Part B covers DME if:
- Your doctor writes a prescription or order.
- The item is medically necessary for a diagnosis or condition.
- It is appropriate for use in the home.
- Its on Medicares DME list and supplied by a Medicare approved vendor.
According to Medicare.govs DME guidance, beneficiaries generally pay 20% of the Medicare approved amount after meeting their Part B deductible, and Medicare pays 80%. That sounds simple until you realize that approved amount is not the sticker price. Ive seen a standard manual wheelchair with a $600 retail price reimbursed at under $200 by Medicare, with the family paying 20% of the $200, not the $600.
Medicare also loves rent to own arrangements. For many items oxygen equipment is a classic example Medicare pays a rental fee for up to 36 months, during which the supplier has to maintain and service the device. After that, you may enter a maintenance period where the supplier still has obligations, but new equipment wont always be automatically provided. Patients are often shocked to find out they don’t own the concentrator sitting in their living room after three years of faithful use.
Where I see the most confusion is around specific categories:
- CPAP/BiPAP: Medicare usually requires a sleep study plus documented usage compliance (often 4+ hours a night on 70% of nights) to keep paying for the machine and supplies.
- Power wheelchairs: Coverage depends heavily on detailed mobility documentation. Ive watched power chair claims get denied simply because the clinic note failed to state the patient couldn’t propel a manual wheelchair safely in the home.
- Hospital beds: Medicare typically covers adjustable beds when the patient needs body positioning that regular beds cannot provide for medical treatment say, severe heart failure, aspiration risk, or decubitus ulcers. Want one for comfort? Medicare will say no.
Medicare Advantage (Part C) plans, which replace traditional Medicare with private coverage, are a different animal. They must cover at least what Original Medicare would, but they can add prior authorizations, restrict you to network DME providers, or offer extra perks. Ive seen one Medicare Advantage plan deny a hospital bed until the family switched to another plan during open enrollment and the second plan approved the same bed in ten days with the same documentation.
Insider Tip (Medicare Billing Specialist): For anything beyond a basic walker or wheelchair, always ask your DME provider before ordering: Is this a capped rental, a purchase, or a mixed model under my specific plan? Don’t assume you’re buying it just because it shows up at your house in a box.
What do other insurers cover?
Commercial insurance plans (employer based or Marketplace) copy Medicares structure but add their own quirks, exclusions, and hoops. One of the biggest myths I hear from families is My plan is great; its PPO, so it will cover everything. That’s not how DME works. The plan can be generous with hospital stays and still be painfully stingy with equipment.
Most commercial plans:
- Use their own list of covered DME, which may be narrower or broader than Medicares.
- Require prior authorization for big ticket items (power chairs, hospital beds, advanced respiratory equipment).
- Set allowed amounts that differ dramatically from Medicares fee schedule.
- May treat some items as rental only while others are purchase only.
In recent years, some plans have moved common items like standard walkers, basic commodes, or inexpensive braces into pharmacy benefits to simplify ordering. Ive seen patients get a walker in 24 hours at a retail pharmacy under their pharmacy card, while the exact same code ordered through a traditional DME channel would have taken two weeks and a prior authorization. If your DME provider tells you an item isn’t covered, its worth asking your insurer whether its available under the pharmacy benefit instead.
Medicaid, especially state Medicaid like Florida’s, is another universe. Coverage is driven by state regulations, waiver programs, and managed care contracts. For example, families using Florida Medicaid for DME quickly learn that what a plan representative promises on the phone and what is actually authorized can be worlds apart. The rules for children may be more generous than adults; certain items may be allowed only under a specific waiver program; and some equipment might be covered only if supplied by a contracted provider in your region.
Then there are developmental disability waivers and home and community based services (HCBS) programs. These can unlock access to highly specialized gear like custom pediatric seating systems or environmental control units that standard Medicaid would never touch. In Florida, for instance, the Developmental Disability Waivers relationship to home medical equipment is often the only path to truly appropriate equipment for adults with lifelong disabilities.
Insider Tip (Care Manager, Commercial & Medicaid Plans): Never trust a single yes, its covered answer from a call center. Always ask for: (1) the policy name, (2) the DME code they’re referring to, and (3) whether prior authorization is required. Then call your DME provider and confirm they agree. If those two sides don’t match, assume there’s a landmine ahead.
How much does DME cost?
The most infuriating truth about DME pricing is that the cash price, Medicare price, and private insurance allowed amount are often three completely different numbers. Ive stood with patients staring at an invoice that might as well be written in code and, in some ways, it is.
To give you ballpark ranges (these are broad national estimates; local vendors in Florida or elsewhere may vary):
- Basic folding walker: retail $50$150; Medicare allowed often <$75.
- Manual wheelchair (standard): retail $400$1,000; Medicare allowed maybe $150$400 depending on region.
- Power wheelchair: retail $2,500$10,000+; allowed amounts vary wildly, often several thousand dollars less than retail.
- Hospital bed (semielectric): retail $800$2,000; frequently handled as a capped rental with a total allowed amount in the same general band.
- CPAP: retail $500$1,200; often billed as rental for 1013 months, with total allowed close to retail but spread out.
- Oxygen concentrator: retail $800$2,000; Medicare usually treats as rental with strict caps and maintenance rules.
Because Medicare and insurers set these allowed amounts, cash pay patients can sometimes do better by negotiating directly with a local provider, especially if you want a higher end or upgraded device. Ive seen a family in Jacksonville negotiate a significant discount on a nicer hospital bed than Medicare would cover, simply because they paid cash through a local hospital bed focused DME supplier. The provider didn’t have to deal with insurance paperwork, so they passed part of the savings along.
There’s also a hidden cost most price lists ignore: service and support. A dirt cheap online wheelchair with no local service contract is often a bad deal once something breaks. An honest local company like a regional provider that offers both DME and specialty needs supplies builds setup, training, maintenance, and emergency repairs into their pricing model, because those things actually matter when you’re trying to live in your house, not a catalog.
From my own vantage point, the smartest families ask two questions every time:
- What will this cost through my insurance, including my share?
- What would it cost if I paid cash, and what support is included either way?
Sometimes the insurance route wins. Sometimes a cash pay arrangement plus a flexible, local vendor is faster, simpler, and not much more expensive especially when your plan applies DME costs to a deductible you’re unlikely to meet anyway.
Insider Tip (DME Company Owner): Ask your DME provider whether the insurance contract actually allows them to offer you a cash option. Some contracts forbid discounting below a certain point. If they say their hands are tied, that’s not always an excuse it might be in writing.
Who pays for DME?
Who pays for DME sounds like a straightforward question. In reality, it is a negotiation between four parties: you, your insurer (if you have one), the government (Medicare/Medicaid), and the supplier. And each one wants to shift as much cost as possible onto the others.
Here’s how it usually breaks out:
- Medicare Part B: Pays 80% of the allowed amount after you meet the deductible; you pay 20%. A Medigap (supplement) may cover that 20%.
- Medicare Advantage: Follows its own cost sharing structure sometimes copays instead of coinsurance, sometimes tiered. You may pay more or less than under Original Medicare.
- Commercial insurance: Applies DME costs to your deductible and then splits with coinsurance (for example, plan pays 70%, you pay 30%) or sets flat copays. High deductible plans can leave you paying full allowed amounts until you hit that number.
- Medicaid: Varies by state. Many Medicaid plans have minimal or no copays for DME, especially for children, but require strict prior authorization.
- Waiver programs: Often pick up costs that regular Medicaid or Medicare wont, particularly for developmental disabilities or long term support needs.
Then there’s the reality of denials and partial approvals. Maybe the plan pays for a basic wheelchair but not the tilt in space version your therapist insists you need. Maybe they’ll fund a semi electric bed but not the fully electric model that would save your caregivers back. In that case, you’re left with three options:
- Accept the covered item.
- Pay an upgrade charge out of pocket if your supplier is allowed to bill one.
- Fight appeal the decision armed with better documentation.
In my own experience, many patients underestimate how elastic these decisions can be when challenged. I once helped a family, whose child had complex seating needs, appeal a denial of a specialized pediatric wheelchair. The initial decision said, blandly, Standard wheelchair is sufficient. After a therapist wrote a detailed letter, attached photos of pressure sores and poor positioning, and cited clinical guidelines summarized by the National Institutes of Health, the same plan reversed itself on second level appeal and approved nearly the entire package.
Another often overlooked payer: workers compensation. If your need for DME is tied to a work injury, the workers comp insurer may be fully responsible for the equipment, including upgrades and long term maintenance. Ive seen workers comp approve equipment in days that would take months under Medicare.
Insider Tip (Health Policy Analyst): The first denial letter is almost always written to sound final. It isn’t. Ask your DME provider to help you read the denial; there is usually a specific phrase or missing detail in the doctors note that you can fix. Appeals with targeted corrections win far more often than people think.
What if I need help with DME?
If you are overwhelmed by all this, you are not the problem. The system is. DME sits at the intersection of medicine, insurance, and logistics, and each side assumes someone else will guide you. In practice, families end up relying on whoever actually answers questions often a front desk person at a clinic or a hurried case manager who has a caseload of 200.
Here are concrete steps I recommend to families:
- Start with your diagnosis, not the device. Ask your doctor, Given my condition and home setup, what equipment will I likely need over the next 612 months? Planning ahead beats scrambling after a fall.
- Get precise prescriptions. Needs wheelchair wont cut it. You want details: type, features, diagnosis codes, and functional limitations.
- Loop in a DME provider early. Ask if they are in network for your plan and which items they expect to be covered vs. self pay.
- Push for case management if your needs are complex. Many health plans offer nurse case managers who can help coordinate multiple DME requests.
- Use community resources. Nonprofits, church programs, loan closets, and disability organizations often have loaner equipment or can help navigate appeal processes.
From a strictly practical standpoint, you want partners who see you as a long term relationship, not a onetime transaction. A provider who also handles specialty needs supplies is more likely to stay engaged as your needs evolve. When your child outgrows an adaptive stroller or your parent transitions from a cane to a walker to a wheelchair, having one team that knows your history is invaluable.
Insider Tip (Home Health Nurse): Invite the DME tech or therapist to actually walk through your home with you doorways, bathrooms, bedroom. The right equipment in the wrong environment is practically useless. Small changes in what you order (wheel size, bed height, transfer devices) can make or break your ability to stay at home.
Conclusion: DME is freedom if you learn how to fight for it
Durable medical equipment is not just a checklist item in your discharge plan; it is infrastructure for your daily life. When we talk about durable medical equipment 101: what it is, what it costs, and who pays for it, were really talking about who gets to decide how independently you live after an injury, diagnosis, or age related decline. The equipment is expensive, the rules are rigid, and the billing codes are intentionally opaque but none of that is a reason to give up and accept whatever the system offers on the first pass.
If there’s one pattern Ive seen again and again, its this: the patients and families who ask specific questions, involve a knowledgeable local provider, and appeal bad decisions end up with better equipment, fewer delays, and lower out of pocket costs. The ones who assume insurance will sort it out are usually the ones calling six weeks after discharge, still sleeping in a recliner because the bed never came. That’s the brutal edge of this system.
So be strategic. Learn exactly what counts as DME. Use Medicares rules to your advantage or work around them with state Medicaid and waiver programs. Compare the real cost of insurance coverage against cash options. And lean hard on providers who actually understand the terrain especially if you’re navigating Florida’s overlapping landscape of Medicare, Medicaid, and developmental disability supports.
Durable medical equipment is, at its core, about agency. You are not a passive recipient of whatever device some unseen reviewer approves. With the right knowledge and the right partners, you can turn a maze of rules into a toolkit and insist on equipment that lets you live at home, on your own terms, for as long as possible.